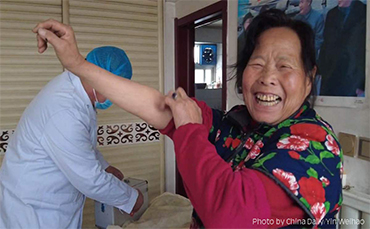



A doctor pays an out-patient visit to check a villager's blood pressures at her home in Tongchuan village, Baoding City, Hebei province. [China Daily/ Yin Weihao]
3. Develop a Large Contingent of Personnel in Rural Medical and Healthcare Services.
3.1 Attract and utilize talented personnel through multiple channels.
Deepen reform of rural medical and healthcare personnel training mechanisms to effectively increase the supply of urgently needed talents in general practice, pediatrics, child healthcare, dentistry, traditional Chinese medicine, nursing, public health, preventive healthcare, mental health, rehabilitation, and occupational health. By 2025, the proportion of certified (assistant) rural doctors (assistant) will be increased to around 45%, and gradually form a rural medical and healthcare service team with certified doctors of general practice.
3.2 Innovate talented personnel utilization mechanism.
Strengthen the integration of allocation and management of county-level healthcare professionals. Where conditions permit, the medical and healthcare professionals recruited should be managed by counties and work in townships or employed by townships and work in villages, and establish a two-way flow mechanism for talented personnel. Coordinate medical and healthcare talents within the county and establish a mechanism of regularly dispatching medical personnel to the countryside. And establish a cross-training system for public health professionals and clinical doctors in medical institutions while encouraging a two-way flow of personnel.
3.3 Improve the income and treatment guarantee mechanism.
Coordinate and balance the relationship between the performance-based salary levels of county-level public hospitals and township-level health centers, and reasonably approve the total amount and levels of performance-based salary. Raise the salary level of general practitioners in rural medical and healthcare institutions to match those of clinicians in county-level public hospitals under the same conditions. Local governments should provide appropriate subsidies to rural doctors serving in impoverished and remote areas as well as in rural revitalization and designated key counties.
3.4 Revitalize the county-level staffing resources.
Dynamically adjust the total number of staff in township health centers every 5 years on a county-by-county basis and make good use of the existing staffing resources. The number of staff for professional and technical personnel in township health centers should not be less than 90% of the total staff.
3.5 Solve retirement and healthcare security issues for rural doctors by category.
Rural doctors who have been included as the staff of public institutions should participate in the basic pension insurance, basic medical insurance for employees and other social insurance of government agencies and public institutions under relevant regulations. Rural doctors who have not been included as the staff of public institutions should participate in relevant social insurance schemes in accordance with relevant regulations, and local governments can provide appropriate subsidies where conditions permit.
4. Reform and Improve the Operation Mechanism for the Rural Medical and Healthcare System.
4.1 Accelerate the construction of a close integrated county-level medical service community.
Promote the construction of a close integrated county-level medical service community, grant the community more autonomy in terms of the use of staffing, personnel recruitment, personnel arrangements, performance assessment, income distribution, professional title evaluation, and other aspects, and promote the implementation of unified management of personnel, funds and property. For the close integrated county-level medical service community, the total amount of payment of medical insurance funds should be implemented, and supervision and assessment should be strengthened as well, an internal supervision and management responsibility system should be established and incentives and constraints should be reinforced.
4.2 Improve the investment mechanism of the rural medical and healthcare system.
Implement the main responsibility of the party committees and governments at the municipal and county level for the construction of the rural medical and healthcare system. The development expenditure of rural medical and healthcare institutions operated by the governments in terms of basic construction and equipment purchase should be fully arranged by the local governments according to the development and construction plan for the primary medical and healthcare institutions. The province should increase coordination efforts to ensure the balanced and healthy development of the rural medical and healthcare system. The central government should support rural medical and healthcare institutions by providing subsidies for basic public health services and the essential drug system.
4.3 Establish and improve the mechanism for cities to support healthy rural development.
Improve the mechanism of urban-rural coordination and rural development supported by urban areas, deepen medical and healthcare paired assistance, plan and implement group-style medical talent assistance, encourage national and provincial-level medical centers to provide paired assistance to the medical and health institutions in the underdeveloped areas, the old revolutionary areas and border areas, and take guiding the grassroots and providing downward services as the basic responsibilities of public hospitals at the county level or above.
5. Improve the Capacity of Medical Guarantee in Rural Areas.
5.1 Consolidate and expand the achievements in poverty alleviation through medical guarantee.
Continuously improve the comprehensive guarantee mechanism of the three-tiered medical services of basic medical insurance, serious illness insurance, and medical assistance. Strengthen the early warning monitoring of high medical expenses and establish a long-term mechanism to prevent and alleviate the risk of poverty caused by illness.
5.2 Increase the support of medical insurance funds.
Reasonably increase the total control indicators of medical insurance funds for rural medical and healthcare institutions, focus on rural medical and healthcare institutions for the annual increase of medical insurance funds, and gradually increase the proportion of medical insurance funds used for rural medical and healthcare institutions in county areas.
5.3 Optimize the service management of rural medical insurance.
Improve the management for services and supervision of medical insurance in the countryside, and explore the integration of village-level medical insurance services into the digital management for a matrix of rural areas.
Source:<http://www.gov.cn/zhengce/2023-02/23/content_5742938.htm>
<http://english.www.gov.cn/policies/latestreleases/202302/24/content_WS63f7ef2cc6d0a757729e7256.html>
Edited and translated by Guo Xinxin